23 Signs You Grew Up With Ehlers-Danlos Syndrome

Growing up with Ehlers-Danlos Syndrome (EDS) is a unique experience that can shape one’s perspective on life in countless ways. This hereditary connective tissue disorder, characterized by joint hypermobility and skin fragility, manifests differently in each individual. However, there are common signs that can indicate a person’s upbringing was influenced by EDS. From early childhood memories to ongoing medical challenges, here are 23 signs you grew up with ehlers-danlos syndrome.
What Is Ehlers-Danlos Syndrome?
Ehlers-Danlos Syndrome (EDS) is a group of genetic disorders that affect the connective tissues in the body. Connective tissues provide support and structure to various organs, blood vessels, skin, and joints. EDS is characterized by abnormalities in the production, processing, or structure of collagen, a major component of connective tissues. Collagen is responsible for the strength and elasticity of the skin, tendons, ligaments, blood vessels, and other structures.
What Causes Ehlers-Danlos Syndrome?
Ehlers-Danlos Syndrome (EDS) is primarily caused by genetic mutations that affect the production or structure of collagen, the main protein in connective tissues. There are several different types of EDS, each resulting from specific genetic abnormalities.
The most common form of EDS, called hypermobile EDS (hEDS), is believed to be inherited in an autosomal dominant pattern, meaning that a person only needs to inherit one copy of the mutated gene from either parent to develop the condition. Other types of EDS follow different inheritance patterns, such as autosomal recessive or X-linked inheritance.
The specific genes involved in EDS can vary depending on the type. Mutations in genes responsible for collagen synthesis or processing, such as COL5A1, COL5A2, COL3A1, or COL1A1, are often implicated in different forms of EDS.
In some cases, EDS may occur sporadically without a clear family history, as new gene mutations can arise spontaneously.
23 Signs You Grew Up With Ehlers-Danlos Syndrome?
Growing up with Ehlers-Danlos Syndrome (EDS) can shape your life in unique ways. Here are 23 signs that indicate you grew up with EDS:
Frequent joint dislocations or subluxations: Your joints would often pop out of place or partially dislocate, leading to instability and pain.
Hypermobile joints: You had the ability to move your joints beyond the normal range of motion.
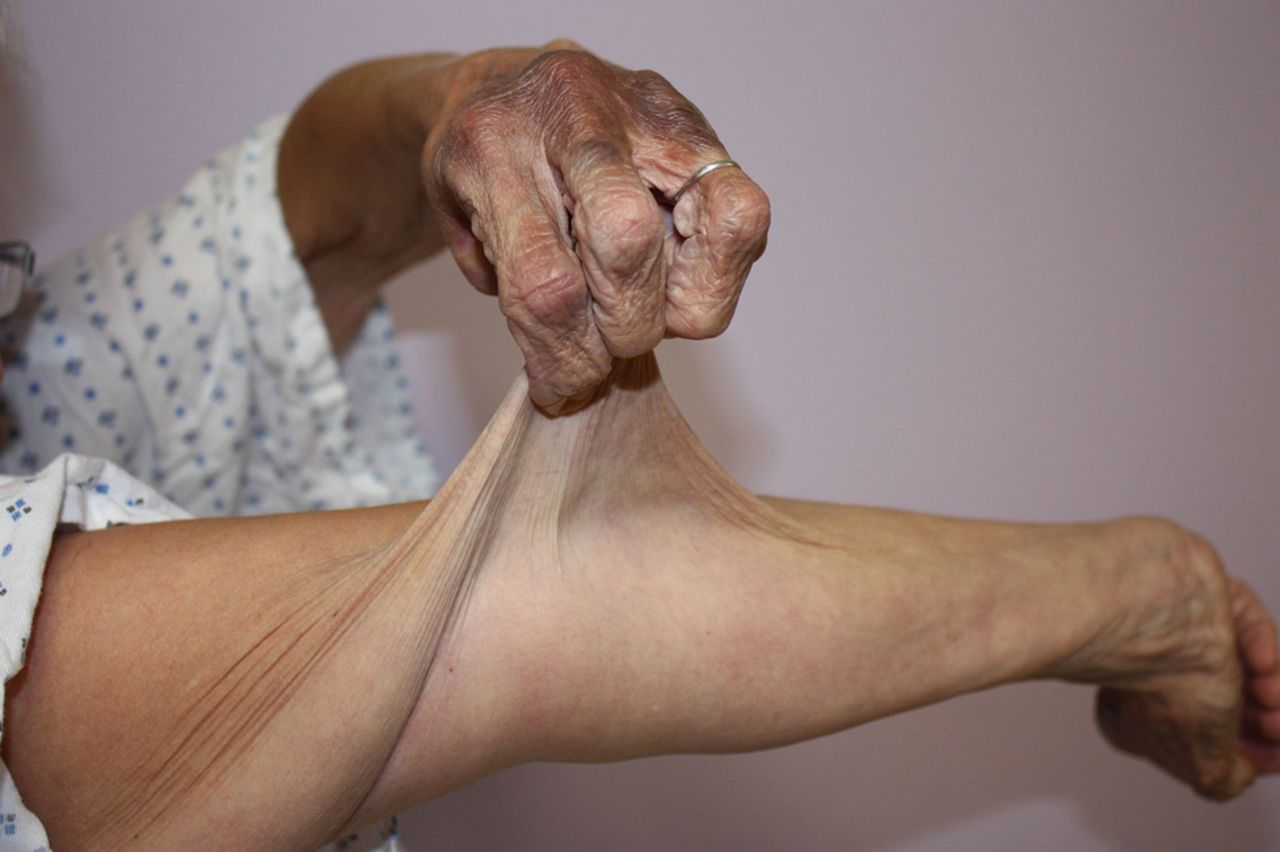
Stretchy and fragile skin: Your skin was elastic, prone to tearing, and easily bruised.
Delayed wound healing: Your wounds took longer to heal compared to others.
Chronic joint and musculoskeletal pain: You experienced persistent pain in your joints, muscles, or bones.
Early-onset arthritis: Despite being young, you developed arthritis or joint degeneration earlier than expected.
Physical limitations: EDS affects your ability to participate in certain physical activities due to joint instability or pain.
Frequent orthopedic interventions: You underwent numerous surgeries or orthopaedic treatments to address joint issues.
Scarring abnormalities: Your scars may have appeared different from others, such as being stretched or atrophic.
Chronic fatigue: EDS often causes persistent fatigue, even with sufficient rest.
Gastrointestinal issues: You experienced digestive problems like acid reflux, irritable bowel syndrome (IBS), or chronic constipation.
Autonomic dysfunction: EDS may have led to dysautonomia, resulting in symptoms like dizziness, rapid heart rate, or blood pressure fluctuations.
Easy bruising: You bruised easily, often with minimal trauma or pressure.
Dental problems: EDS contributed to dental issues like enamel defects, gum disease, or temporomandibular joint (TMJ) disorders.
Fragile blood vessels: Your blood vessels were more prone to rupture, leading to conditions like varicose veins or easy bleeding.
Scoliosis or spinal abnormalities: EDS could have affected your spine, causing curvature (scoliosis) or other structural issues.
Stretchy or hyperextensible skin: Your skin could be stretched further than normal, and you may have demonstrated party tricks like skin pinching or folding.
Chronic headaches: You experienced frequent or chronic headaches, including migraines.
Joint bracing or support: You regularly used braces, splints, or other supports to stabilize your joints.
Multiple medical specialists: You saw various specialists, such as rheumatologists, orthopedic surgeons, or dermatologists, to manage your condition.
Difficulty with physical education or sports: EDS limits your ability to fully participate in physical education classes or engage in certain sports.
Adaptations and accommodations: Growing up, you had to make adjustments and accommodations in daily life to manage EDS-related challenges.
Support groups or online communities: You sought support and connection with others who shared similar experiences through EDS support groups or online platforms.

What Are The Treatments Of Ehlers-Danlos Syndrome?
Here are some common approaches used in the management of EDS:
Multidisciplinary care
EDS often requires a team of healthcare professionals, including geneticists, rheumatologists, orthopedic specialists, physical therapists, occupational therapists, pain management specialists, and other specialists based on specific symptoms.
Pain management
Chronic pain associated with EDS may be addressed through a combination of medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs), pain relievers, and in some cases, opioids. Physical therapy, occupational therapy, and complementary therapies like acupuncture or transcutaneous electrical nerve stimulation (TENS) may also help manage pain.
Physical therapy and exercise
A customized exercise program supervised by a physical therapist can help strengthen muscles, improve joint stability, and enhance overall physical function. Low-impact exercises, such as swimming or cycling, are often recommended to minimize joint stress.
Joint protection and bracing
Assistive devices like braces, splints, or orthotics can provide support, stabilize joints, and prevent frequent dislocations or subluxations.
Wound care
Special attention should be given to wound care due to delayed healing. Proper wound cleaning, dressings, and early intervention for infections or complications are essential.
Gastrointestinal management
Dietary modifications, medications, and lifestyle changes can help manage gastrointestinal symptoms such as acid reflux, IBS, or constipation. Working with a registered dietitian or gastroenterologist can be beneficial.
Cardiac monitoring
Regular cardiac evaluations and monitoring may be necessary for individuals with EDS types that involve cardiovascular complications. This helps detect and manage conditions like mitral valve prolapse or aortic dilation.
Psychological support
Living with a chronic condition like EDS can have a significant impact on mental health. Accessing psychological support through therapy or support groups can be valuable in coping with the emotional and psychological aspects of the condition.
When To See A Doctor For Ehlers-Danlos Syndrome?
If you suspect you have Ehlers-Danlos Syndrome (EDS) or experience symptoms like joint hypermobility, chronic pain, or fragile skin, it is recommended to see a doctor for evaluation and proper diagnosis. Early detection and appropriate management can help improve your quality of life and prevent potential complications.

Conclusion
In conclusion, recognizing the 23 signs you grew up with Ehlers-Danlos Syndrome (EDS) is not just about identifying the physical manifestations of this rare genetic disorder. It’s about understanding the lifelong challenges and adaptations that individuals with EDS face. These signs encompass a wide range of symptoms, from hypermobility and joint pain to digestive issues and skin fragility. More importantly, they signify resilience and determination in the face of adversity.
Frequently Asked Questions
Q1: What are common symptoms of EDS?
Ans: Symptoms can include joint hypermobility, skin fragility, chronic pain, and easy bruising.
Q2: How is EDS diagnosed?
Ans: Diagnosis involves a clinical evaluation, family history assessment, genetic testing, and physical examination.
Q3: What treatments are available for EDS?
Ans: Treatment focuses on managing symptoms and may include pain management, physical therapy, and lifestyle modifications.
Q4: Is EDS a progressive condition?
Ans: Some types of EDS can be progressive, meaning symptoms may worsen over time, while others remain stable.
Q5: Can EDS be life-threatening?
Ans: Certain types of EDS, particularly those affecting blood vessels or the heart, can pose life-threatening risks.